
WHAT IS A DIGITAL FRONT DOOR?
The phrase “digital front door” refers to giving patients and caregivers access via online and mobile communication channels. The idea is that, even though many services must still be provided in person, patients can go through the “front door” before they've physically arrived. Services that tend to be part of a digital front-door strategy are: schedule requests, check-ins, health triage, registration, video visits, and prescription refills.
What many haven't realized is that there are 3 prerequisites to a successful digital front door.
FEDERAL & MARKET PRESSURES
Understandably, COVID increased the demand for digital front-door capabilities in all industries, particularly healthcare.
Because of the pandemic, CMS increased telehealth reimbursements. Even for traditional providers, copays are smaller and often waived. In fact, some audio-only visits are reimbursed at the same rate!
Patient demand for digital front door access has been substantial. An increase in telehealth has meant
![]() More telephone calls
More telephone calls
![]() More website visits
More website visits
![]() More SMS messaging
More SMS messaging
![]() More patient portal use
More patient portal use
![]() More video chats
More video chats
INITIAL INVESTMENTS AREN’T WORKING
While telehealth and digital front-door demand skyrocketed, provider satisfaction with telehealth has plummeted. We predict 2021 will be the Year of Telehealth Burnout.
Within the last 2 decades, we’ve seen retail and online financial services mature; it is now easy to conduct many services that would have required going into a store or a bank. Healthcare has to go through this same transformation.
SIGNS YOU HAVE A DIGITAL FRONT-DOOR PROBLEM
1. Did patient usage of telehealth, website, and telephone spike, only to sharply drop shortly thereafter?
A lot of telehealth usage trends looked something like this:
.png?width=1493&name=image-png-4%20(1).png)
If patients are struggling with the experience, they won’t keep coming back.
2. Do patients have to log in to request an appointment or download forms?Bad designs like this can cost millions.
3. Can patients schedule any appointment themselves on their mobile phone day or night?"If not, don’t even bother offering “online scheduling.”
4. Can callers talk to one person for a lab report, bill payment, prescription refill, or immunization form?Having to wait for callbacks or passed between agents is a major source of patient dissatisfaction.
5. Do your staff use more than 2 tools when helping patients?You can only streamline the experience for patients once you’ve streamlined the experience for staff.
WHY IS THERE A PROBLEM?
Healthcare consists of a large number of individual services delivered by different people using a variety of tools.
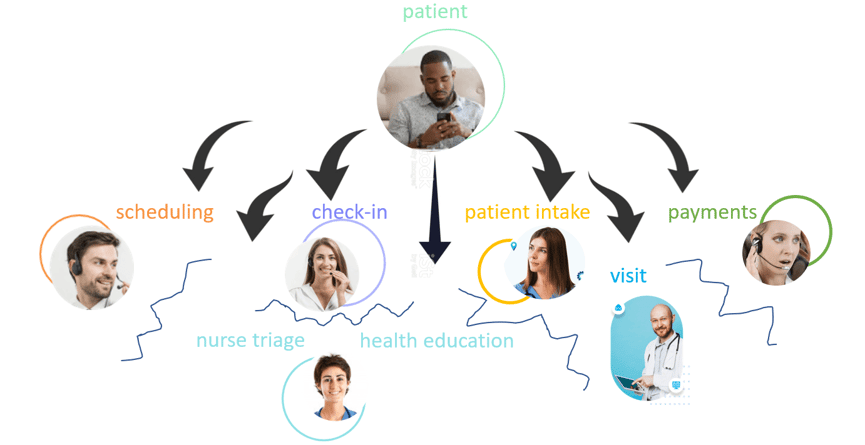
Opening the digital front door doesn’t automatically resolve this segmented service structure.
Fracturing is unavoidable with traditional tools because all these roles are necessary, separate, and complex. For example, here is more detail on just the scheduler's tasks and tools:
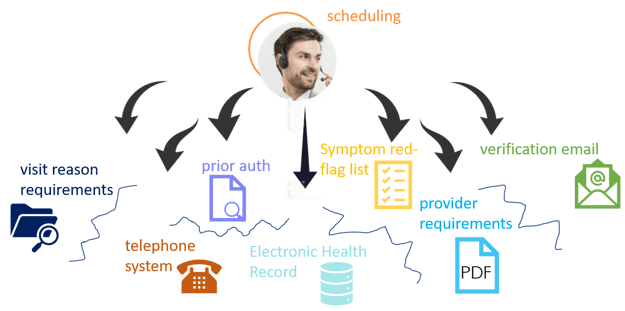
Before working with Care Desk, a typical Keona client used 5-8 different applications just to schedule an appointment! The workflow is so complicated, training could go as long as six weeks and it would be half a year before they would not make mistakes!
See The Only 3 Ways to Reduce Scheduling Errors
Fracturing goes far beyond digital access issues and has been a core problem for some time. According to a 2019 research brief by Altarum, travel and wait times for healthcare are longer than wait times for legal, insurance, or government services such as licensing!
If you’ve invested in digital front-door technology, chances are it is about as effective as

CREDIT: WARNER BROS. & VITAGRAPH STUDIOS
LEARNING FROM PAINFUL EXPERIENCE
Keona Health made this mistake ourselves. Our first product was a digital front door app that allowed patients to ask questions and it would auto-ask follow-ups. When we went to market, we initially made good sales… and then the product failed.
Why? The same reason that causes others to fail – provider infrastructure was not sophisticated enough to support it. Patients would submit their request and support would kick in. However, nurses and providers would not respond until almost 24 hrs later! Patients were “impatient" if you will and the service got zero repeat users.
THE 3 PREREQUISITES TO SUCCESS
We’ve learned a lot from repeated failures. What we’ve learned is that much of healthcare is missing the building blocks for excellent service. Here are core capabilities that need to be developed:
 A single system to track, time, and prioritize all requests
A single system to track, time, and prioritize all requests
Most organizations don’t know how long a patient’s request has been waiting. They tackle issues in the order they came in without any indication until the read the request or listen to the voice message if the patient’s request is urgent or emergent. They have little data on what percent of requests are for what issues or how many questions were going to which care team, or how efficient each team is in processing.
 A single system to document and organize the workflows and consolidate the data sources.
A single system to document and organize the workflows and consolidate the data sources.
Workflows are fractured into different silos and often only understood through tribal knowledge. “Tribal knowledge” is knowledge gained by doing the work. It is not documented or analyzed. Tribal knowledge is often assumed or seen as simple and obvious, when in fact it is complicated and multi-faceted. Neither the people who manage nor the people who perform the jobs could outline all the workflows.The corollary to this is that too many tools are being used. This leads to complexity, lost time, and data entry errors as users jump from one tool to another.
 Automation for complicated workflows
Automation for complicated workflows
Most healthcare workflows are very complicated. The triage nurse has to assess the patient, help the patient reach a disposition, educate and advise, page/message the physician, and document the symptoms, disposition, and care advice in the patient’s chart. The scheduler has to determine the visit type, screen patient symptoms for urgency, select/validate insurance, search the calendar for slots that match what the patient can attend, check the provider visit requirements for the slot they find, schedule the appointment and document the reasons. In cases of urgent or emergent issues they need to forward to a nurse or page a provider. Similar complexity exists for care coordinators, doctors, radiologists. These processes are ripe for automation and business logic to increase consistency and decrease time.
Only once these things are in place will the digital front door be an easy and smooth experience for patients.
We have taken clients who already had “online scheduling” from a process for a visit with symptoms to a referral goes like this:
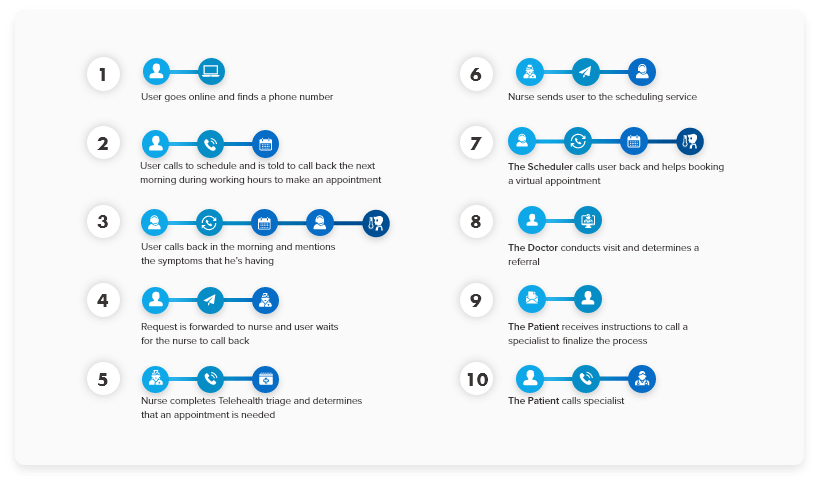
After process redesign and automation, that same scenario is reduced to a few steps:
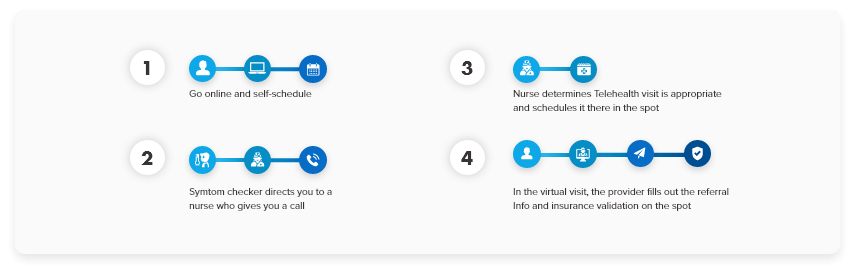
WHAT YOU SHOULD DO
-
Next, check out Keona’s Patient Service Maturity Model
-
Learn more about how an automated contact center using one tool to automate calls, scheduling, safety, and triage can increase revenue and save time
About Keona Health
At Keona Health, we believe that relationships matter. We know that a clinic’s triage system can test a patient-doctor relationship, especially if a patient cannot easily get the help he or she is seeking. Keona Health offers healthcare software and automation solutions to ease the burden of telephone triage on medical practices and help medical professionals better communicate with patients.
How We Turned the Challenge Into Results
Posted By

Stephen Dean is COO of Keona Health, where he’s spent 13 years building AI systems that transform patient access. Before “agentic AI” was a term, his team was deploying autonomous systems that now handle millions of patient conversations annually.
Related Post
November 19, 2024
heading into 2025, healthcare organizations face increasing pressure to digitize...
October 18, 2023
is your healthcare call center getting crushed under the weight of frustrated...

.png?width=74&name=Self-Scheduling-Featured1%20(1).png) But there is a better way.
But there is a better way.

